The Intensive Care Unit (ICU) is the area with the highest nursing density and most stringent monitoring requirements in a hospital. Each patient in the ICU requires multiple vital sign monitoring, continuous treatment, and frequent nursing procedures, all of which demand a sustained investment of time and professional effort from the nursing team.
Meanwhile, the key equipment in the ICU—the electric ICU bed—not only provides positioning and safety for critically ill patients but also directly impacts the efficiency and methods of nursing care. Because of these extremely high nursing demands, a crucial question arises: how many nurses are needed per electric ICU bed?
In the healthcare industry, this question involves nursing safety, staffing, scientific management, and clinical nursing standards.
While staffing levels vary slightly across different countries and institutions, generally speaking, the nurse staffing standards for ICUs are relatively consistent, tailored to the severity of the patient's condition, the intensity of the nursing workload, and the complexity of equipment use.

Why is the nursing ratio higher for electric ICU beds?
To understand how many nurses are needed per electric ICU bed, it's crucial to first recognize that the nursing needs of ICU patients are entirely different from those of patients in general wards. The nursing tasks in the intensive care unit (ICU) include not only routine care but also the management of numerous highly complex and continuous life support procedures.
Electric ICU beds exist to assist medical staff in performing these tasks, such as positioning, turning, suctioning, respiratory therapy, and managing intravenous lines; however, they do not reduce the inherent difficulty of nursing care. On the contrary, due to the generally critical condition of ICU patients, the number of nurses must be higher than in other departments.
Therefore, electric ICU beds are not a basis for reducing the number of nurses, but rather an important tool to help nurses perform their work more efficiently.
The reasons for the high nurse-to-patient ratio include:
1. Unstable vital signs in ICU patients require real-time monitoring.
2. Frequent medical procedures, such as suctioning, turning, and managing various tubes.
3. Frequent use of equipment such as ventilators, CRRT, and infusion pumps.
4. A large number of operations involving the functions of the electric ICU bed require specialized personnel.
5. The need to respond to emergencies at any time.
These characteristics dictate that each electric ICU bed requires more nurses to provide continuous, professional, and safe care.
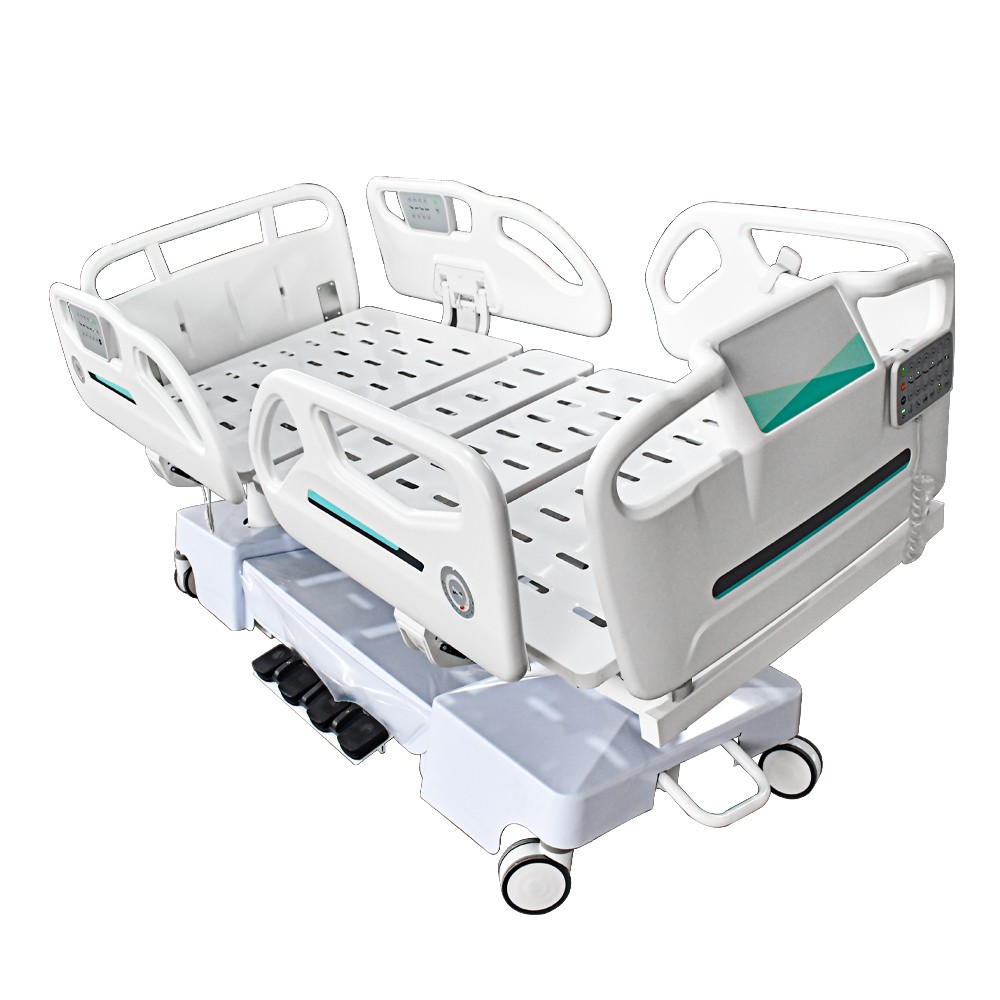
How many nurses are typically needed for one electric ICU bed?
From a nursing and critical care medicine perspective, while different countries have different standards, generally speaking, the nurse-to-bed ratio in intensive care units (ICUs) falls within the following range:
Each electric ICU bed requires one nurse to provide full-time care (1:1) or one nurse to care for two beds (1:2).
That is:
• Nursing ratio 1:1 (one nurse for one electric ICU bed)
• Nursing ratio 1:2 (one nurse for two electric ICU beds)
These two ratios are the most common, both internationally and in industry consensus.
This means that each electric ICU bed requires at least 0.5–1 nurses.
What factors affect the number of nurses needed per bed?
Nursing staffing must be flexibly adjusted according to the ward's situation. The main factors leading to different nursing staff numbers per electric ICU bed include:
How does the severity of an ICU patient's condition affect the nursing ratio?
The more critical the patient's condition, the higher the nursing needs. For example:
• Use of a ventilator
• Use of continuous bedside monitoring
• Dependence on sedation or analgesia
• Requirement of frequent suctioning
• Multiple intravenous lines
• Requirement of continuous position management
• High-risk adverse events (cardiac arrest, aspiration, etc.)
In these situations, almost every electric ICU bed must be managed independently by one nurse.
The more severe the patient's condition, the closer the nurse-to-patient ratio becomes to 1:1.
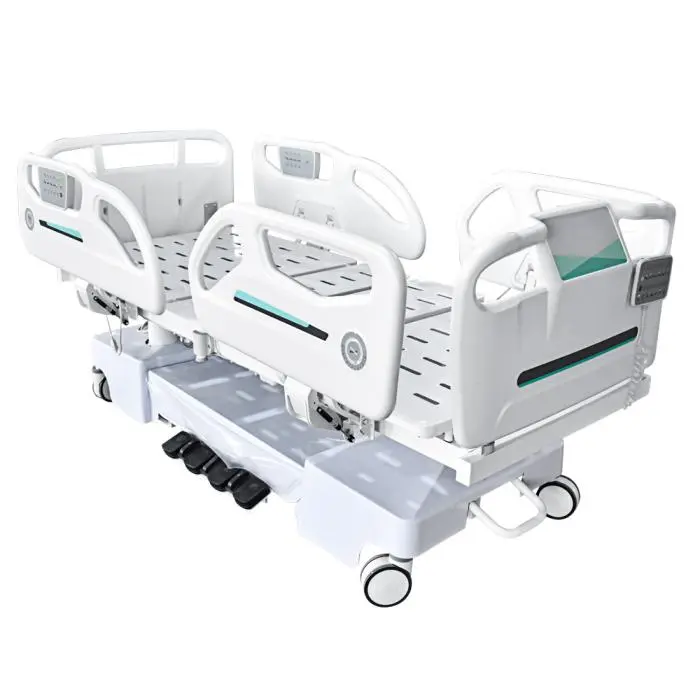
Do the functions of the electric ICU bed itself change the nursing needs?
Although electric ICU beds have multiple functions, such as:
• Backrest adjustment
• Legrest adjustment
• Lateral tilting and turning
• Trending position, counter-trending position
• Cardiac chair position
• One-button reset
These functions do help nurses reduce physical exertion and improve efficiency, but they do not reduce the frequency of nursing actions themselves.
For example:
• Patients still require frequent turning.
• Vital signs still need monitoring.
• Bed repositioning still needs to be adjusted to improve breathing.
• Pressure ulcer risk still needs to be assessed.
• Equipment management and wiring maintenance still require attention.
Therefore, electric ICU beds are more about speeding up processes than reducing the number of nursing staff.
How does the complexity of nursing tasks affect the number of nurses per bed?
ICU nursing tasks include:
• Tubing management
• Medication adjustment
• ECG monitoring
• Intake and output recording
• Skin care
• Indicator assessment
• Equipment operation
• Positioning and turning
• Infection risk control
These tasks are not only time-consuming but must be performed at the right time. If nurses are responsible for too many beds, they will not be able to complete all nursing tasks in a timely manner.
Therefore, in wards with heavy nursing workloads, each electric ICU bed typically requires one nurse (1:1).
Why do patients in the acute phase need more nurses?
Patients in the acute phase experience rapid changes in condition, such as:
• Acute respiratory failure
• Multiple organ dysfunction
• Immediate postoperative monitoring
• Severe infection
• Hemodynamic instability
During this phase:
• Nurses need to continuously monitor bedside equipment
• Electric ICU beds require more frequent position adjustments
• The nursing team needs to be prepared to respond to emergencies at any time
Therefore, patients in the acute phase often require:
• One nurse per electric ICU bed (1:1 ratio)
And sometimes additional support staff are needed.
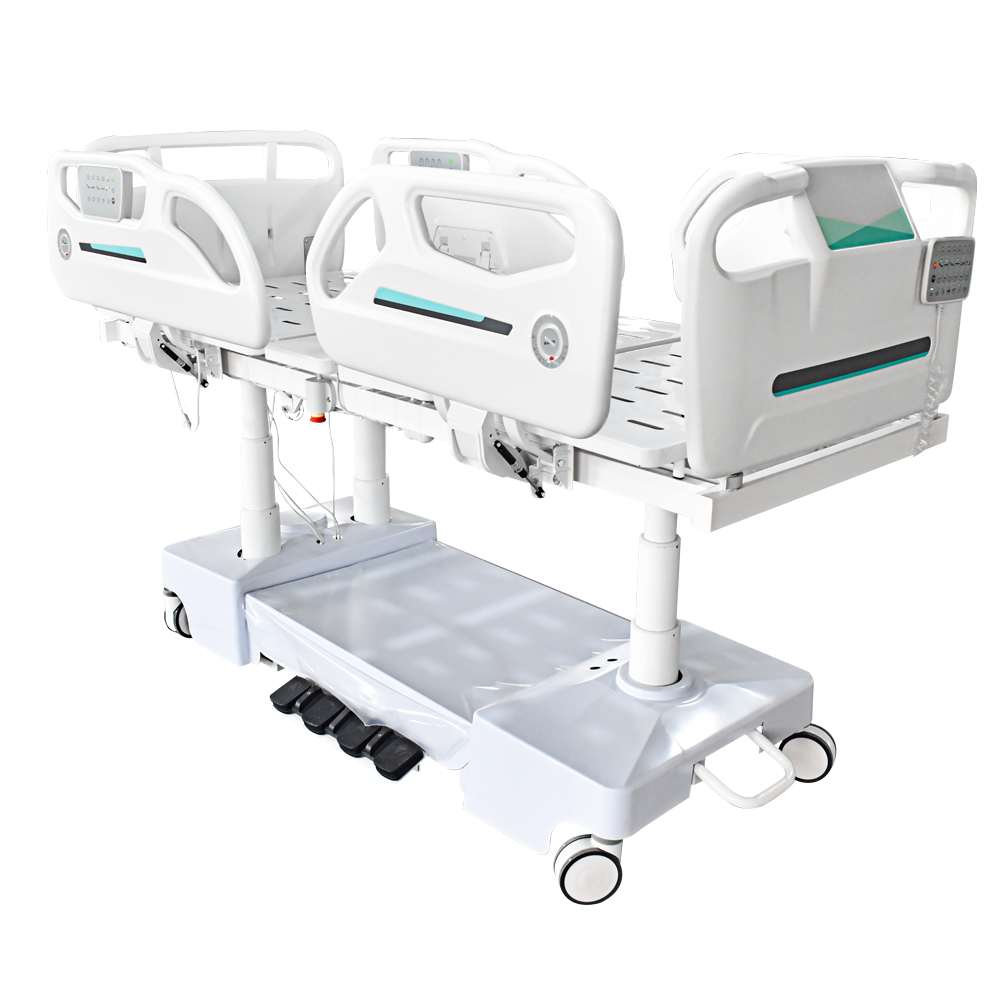
Why shouldn't the number of nurses be determined solely by the number of beds?
While this article discusses "how many nurses are needed per electric ICU bed," a core principle in actual nursing management is: The number of nurses should be determined by the patient's nursing needs, not the number of beds.
Reasons for this difference include:
1. Beds may be vacant, but nursing staff must be kept at a minimum
ICUs are not always full, but a certain number of nurses are needed on-site to handle critically ill patients who may be admitted at any time.
2. Different Patients Have Different Nursing Needs
Even with the same electric ICU bed, some patients can breathe semi-spontaneously, while others require ventilator support; their nursing needs are completely different.
3. Nursing Task Intensity Varies at Different Times
For example:
• Shift Change
• Doctor's Order Execution Time
• Peak Nursing Procedure Time
All require more nurses.
Therefore, the number of beds is merely the number of devices; nursing staffing must be determined based on complexity, not simply "beds × ratio".
Why do electric ICU beds significantly impact nurses' work efficiency?
While electric ICU beds cannot reduce the number of nurses, they can significantly improve nursing efficiency:
1. Reduced Physical Exertion from Turning Patients
The tilting function makes it easier for nurses to help patients turn over.
2. Improved Posture for Respiratory Therapy
Backrest Adjustment helps patients achieve the optimal breathing posture.
3. Increased Emergency Efficiency
The one-button reset function allows for instant bed adjustment to a CPR position.
4. Smoother Nursing Procedures
Bed height adjustment improves operating height, reducing back injuries.
Because electric ICU beds can improve efficiency, nurses can manage multiple nursing tasks more scientifically, thereby ensuring the quality of care for each bed.

